TL;DR
Hemoglobinuria is the presence of free hemoglobin in urine, distinct from hematuria (whole RBCs). It occurs when intravascular hemolysis overwhelms the body’s hemoglobin-handling capacity (haptoglobin, hemopexin).
- Causes ▾: Transfusion reactions, hemolytic anemias (PNH, G6PD deficiency, AIHA, MAHA), mechanical hemolysis, infections (malaria), and certain toxins/drugs. Rhabdomyolysis can also lead to hemoglobinuria (though primarily myoglobinuria).
- Symptoms ▾: Red/brown urine, fatigue, jaundice, pain, and symptoms related to the underlying cause.
- Diagnosis ▾: Urine analysis (positive for blood, few/no RBCs), blood tests (CBC, LFTs, haptoglobin), and specific tests for underlying conditions.
- Differential diagnosis ▾: Hematuria, myoglobinuria, porphyria, and drug-induced urine discoloration.
- Treatment ▾: Address the underlying cause and providing supportive care (hydration, electrolyte management).
- Complications ▾: Acute renal failure, chronic kidney disease, DIC, and iron overload.
*Click ▾ for more information
Introduction
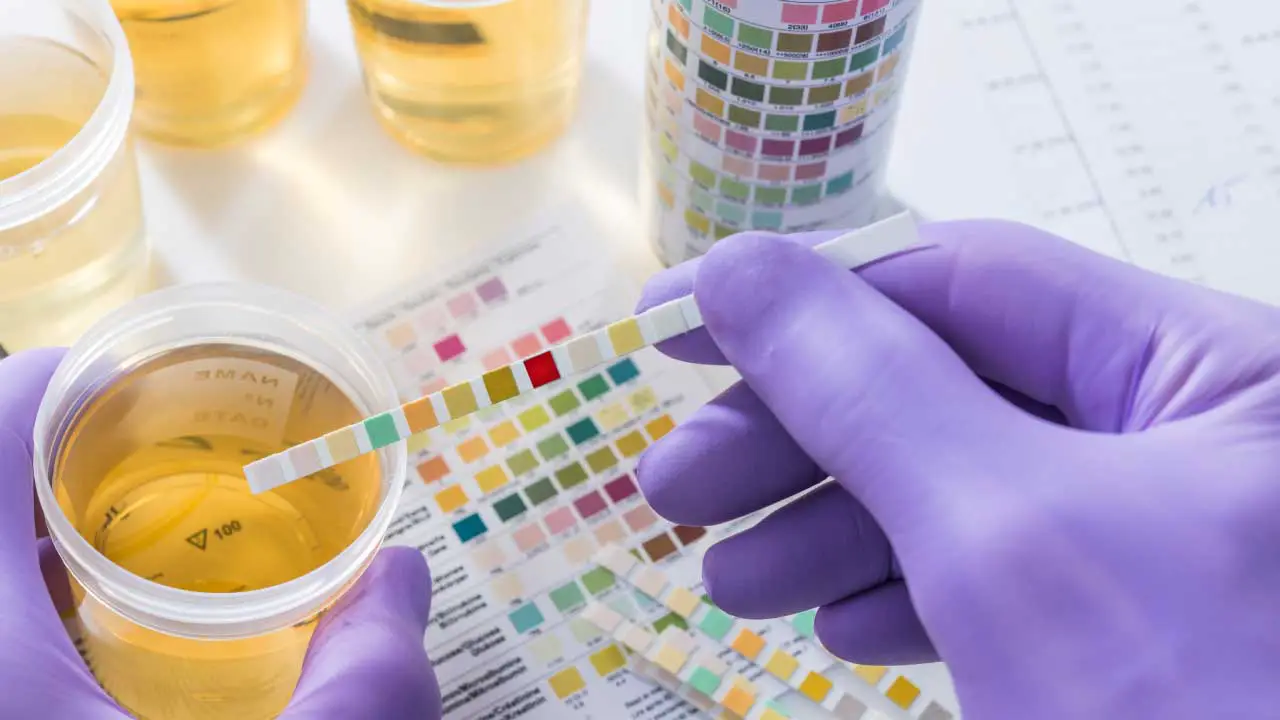
Hemoglobinuria is the presence of free hemoglobin in the urine. This occurs when red blood cells break down within the bloodstream (intravascular hemolysis), releasing hemoglobin into the plasma. The kidneys then filter this excess hemoglobin, which is excreted in the urine, often causing a reddish-brown discoloration.
What is the difference between hematuria and hemoglobinuria?
Hematuria refers to the presence of whole red blood cells in the urine. The urine may appear red or pink, and microscopic examination will reveal the presence of intact red blood cells. Causes of hematuria often relate to problems within the urinary tract, such as infections, kidney stones, or trauma.
Hemoglobinuria involves the presence of free hemoglobin (the protein within red blood cells) in the urine, not the red blood cells themselves. The urine may also be discolored, but microscopic examination may show very few or no red blood cells. It signifies that red blood cells are being destroyed within the blood vessels.
What is free hemoglobin in urine?
Normally, when red blood cells reach the end of their lifespan, they are broken down primarily in the spleen. However, in certain conditions, red blood cells rupture within the bloodstream (intravascular hemolysis). This releases hemoglobin into the plasma. Following the release of hemoglobin from broken-down red blood cells, it undergoes metabolic processing where the globin protein is separated and degraded into recyclable amino acids, while the heme component is further metabolized.
Haptoglobin, a protein in the blood, normally binds to this free hemoglobin, preventing it from being filtered by the kidneys. Hemopexin is a protein that binds to free heme, preventing it from causing oxidative damage. The heme-hemopexin complex is also taken up by the liver.
However, when the capacity of haptoglobin and hemopexin is exceeded, or in cases of massive intravascular hemolysis, the free hemoglobin level in the plasma rises significantly. This overwhelms the kidneys’ reabsorption capacity. Thus, the excess free hemoglobin is filtered by the glomeruli and appears in the urine, resulting in hemoglobinuria.
It is important to understand that the presence of free hemoglobin in the urine indicates that there has been destruction of red blood cells within the blood vessels. This is a very different process than red blood cells leaking into the urine from the urinary tract.
What is the clinical significance of hemoglobinuria?
Recognizing hemoglobinuria is crucial because it signals that red blood cells are being destroyed within the bloodstream (intravascular hemolysis) or that there’s significant muscle breakdown (rhabdomyolysis). This process isn’t normal and points to underlying pathological conditions, ranging from potentially life-threatening transfusion reactions and severe infections like malaria to hemolytic anemias and muscle injuries.
Early detection through urine analysis can prompt timely investigations and interventions, preventing serious complications such as acute renal failure and systemic organ damage.
Causes of Hemoglobinuria
Hemoglobinuria arises from conditions that lead to the presence of free hemoglobin in the urine. These conditions can be broadly categorized into intravascular hemolysis and rhabdomyolysis, with other less common causes also contributing.
Intravascular Hemolysis

- Transfusion Reactions
- ABO Incompatibility: This is a severe, life-threatening reaction where transfused blood is incompatible with the recipient’s blood type, causing immediate and massive RBC destruction.
- Delayed Hemolytic Transfusion Reactions: These occur days or weeks after a transfusion due to antibodies against minor blood group antigens.
- Hemolytic Anemias
- Paroxysmal Nocturnal Hemoglobinuria (PNH): A rare acquired stem cell disorder where RBCs are abnormally susceptible to complement-mediated lysis.
- Glucose-6-phosphate Dehydrogenase (G6PD) Deficiency: An inherited enzyme deficiency that makes RBCs vulnerable to oxidative stress, leading to hemolysis after exposure to certain drugs, foods, or infections.
- Autoimmune Hemolytic Anemia (AIHA): The body’s immune system mistakenly attacks its own RBCs.
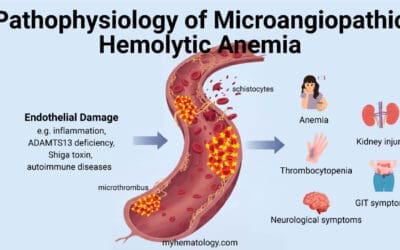
- Microangiopathic Hemolytic Anemia (MAHA): RBCs are damaged as they pass through narrowed or damaged small blood vessels, as seen in conditions like thrombotic thrombocytopenic purpura (TTP) and hemolytic uremic syndrome (HUS).
- Mechanical Hemolysis
- Artificial Heart Valves: The shear stress from mechanical heart valves can damage RBCs.
- Strenuous Exercise (March Hemoglobinuria): Repetitive impact during intense exercise can cause RBC damage.
- Severe Burns: Thermal injury can directly damage RBCs.
- Infections
- Malaria (especially Plasmodium falciparum): The parasite invades and destroys RBCs.
- Clostridial Sepsis: Certain Clostridium species produce toxins that cause massive RBC lysis.
- Toxins and Drugs
- Certain snake venoms.
- Drug-induced hemolytic anemia from certain medications.
Rhabdomyolysis
Muscle breakdown releases myoglobin into the bloodstream. While myoglobinuria is the more accurate term, significant rhabdomyolysis can also result in hemoglobinuria. These can be caused by crush injuries, excessive exercise and certain medications e.g. statins.
Less Common Causes
- Severe burns: In addition to mechanical damage, burns can trigger other hemolytic pathways.
- Renal infarction: Though less common, if the infarction is severe enough, it can cause hemoglobin to be present in the urine.
Signs and Symptoms of Hemoglobinuria
The clinical presentation of hemoglobinuria can vary significantly depending on the underlying cause and the severity of the condition. The severity of these symptoms can range from mild to life-threatening, depending on the extent of hemolysis and the underlying pathology.
- Macroscopic Hemoglobinuria: The most prominent sign is a noticeable change in urine color. It can appear red, brown, or even black, resembling the color of cola.
- Associated Symptoms
- Anemia-related symptoms
- Fatigue and weakness: Due to the loss of red blood cells.
- Pallor: Pale skin due to reduced hemoglobin levels.
- Shortness of breath.
- Increased heart rate.
- Jaundice: Yellowing of the skin and eyes, indicating increased bilirubin levels from red blood cell breakdown.
- Pain
- Abdominal or back pain, which can be associated with kidney involvement or underlying conditions like hemolytic anemia.
- Muscle pain and weakness: Especially in cases of rhabdomyolysis.
- Fever and chills: These can occur in cases of infectious causes, such as malaria or clostridial infections.
- Other symptoms: Symptoms related to the specific underlying cause, such as those from a transfusion reaction, or symptoms related to paroxysmal nocturnal hemoglobinuria (PNH). In cases of PNH there can also be increased risk of blood clotting.
- Anemia-related symptoms
Laboratory Investigations
Laboratory investigations are crucial for confirming the presence of hemoglobinuria, identifying its underlying cause, and assessing the extent of organ damage.
Urine Analysis
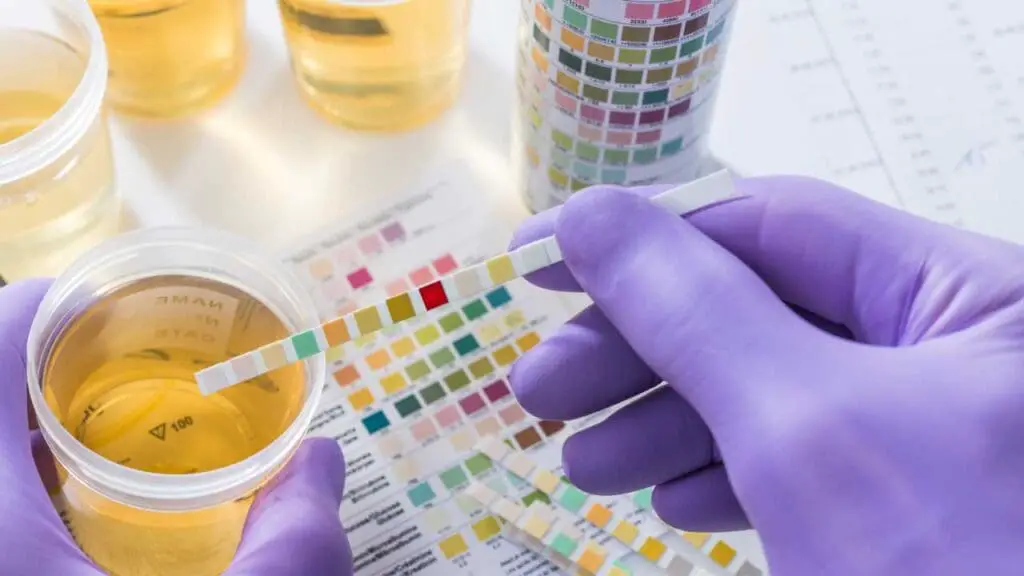
- Dipstick Testing: This is a rapid screening test that detects the presence of blood (hemoglobin or myoglobin) in the urine. It’s important to note that a positive dipstick test can’t distinguish between hemoglobinuria and myoglobinuria.
- Microscopic Examination of Urine Sediment: This is important as it helps differentiate between hematuria and hemoglobinuria. In hemoglobinuria, few or no red blood cells are typically seen in the urine sediment, while in hematuria, red blood cells are abundant.
- Distinction Between Hemoglobinuria and Myoglobinuria: This can be difficult with dipstick testing alone. The clinical context (e.g., recent muscle injury, strenuous exercise) of the patient is important. Sometimes, specific lab tests for myoglobin are performed.
Blood Tests
- Complete Blood Count (CBC): To assess the degree of anemia and to evaluate bone marrow response to red blood cell destruction (increased in hemolysis).
- Liver Function Tests (LFTs): Increased bilirubin levels due to red blood cell breakdown and elevated lactate dehydrogenase (LDH) levels in hemolysis.
- Haptoglobin Levels: Decreased in intravascular hemolysis, as haptoglobin binds to free hemoglobin and is removed from circulation.
- Coombs Test (Direct and Indirect): To detect autoimmune hemolytic anemia (AIHA).
- Glucose-6-Phosphate Dehydrogenase (G6PD) Fluorescent Spot Test Glucose-6-phosphate Dehydrogenase (G6PD) Enzyme Activity: To diagnose G6PD deficiency.
- Paroxysmal Nocturnal Hemoglobinuria (PNH) Testing: Flow cytometry to detect the absence of CD55 and CD59 on red blood cells.
- Renal Function Tests: Creatinine and blood urea nitrogen (BUN) levels to assess kidney function and detect acute kidney injury.
Additional Investigations (Based on Suspected Cause)
- Blood Cultures: To identify bacterial infections, such as clostridial sepsis.
- Malaria Smear or Rapid Diagnostic Tests: To diagnose malaria.
- Imaging Studies (e.g., Ultrasound, CT Scan): To assess for kidney damage, organ involvement, or other underlying pathologies.
- Coagulation studies: To assess for Disseminated intravascular coagulation (DIC).
Differential Diagnosis of Hemoglobinuria
| Condition | Key Distinction | Clinical/Lab Findings | Causes |
| Hematuria | Presence of intact red blood cells in urine. | Red or pink urine. Microscopic: numerous RBCs in urine sediment. | Kidney stones. Urinary tract infections. Tumors. Trauma. |
| Myoglobinuria | Presence of myoglobin (muscle protein) in urine. | Urine dipstick positive for blood. Clinical: muscle pain, recent trauma, strenuous exercise. Specific lab: elevated myoglobin. | Crush injuries.Rhabdomyolysis.Excessive muscular activity. |
| Porphyria | Disorders affecting heme synthesis, leading to porphyrin accumulation. | Discolored urine.Abdominal pain, neurological problems, photosensitivity.Specific lab: elevated porphyrins. | Inherited enzyme deficiencies. |
| Drug-Induced Urine Discoloration | Urine discoloration caused by certain medications. | Variable urine color.Negative urine dipstick for blood. Medication history positive. | Rifampin. Beets. Other medications. |
| Concentrated Urine | Increased urine solutes, that darkens urine color. | Urine is very dark, and urine dipstick is negative for blood. | Dehydration |
General Treatment and Management of Hemoglobinuria
The treatment and management of hemoglobinuria focus on addressing the underlying cause, preventing complications, and providing supportive care.
Addressing the Underlying Cause
- Treatment of Infections
- Antibiotics for bacterial infections (e.g., clostridial sepsis).
- Antimalarial drugs for malaria (especially Plasmodium falciparum).
- Management of Hemolytic Anemias
- Transfusions: To replace lost red blood cells.
- Corticosteroids: For autoimmune hemolytic anemia (AIHA).
- Immunosuppressants: For severe AIHA or other autoimmune conditions.
- Eculizumab or ravulizumab: For paroxysmal nocturnal hemoglobinuria (PNH).
- Avoidance of triggering factors for G6PD deficiency.
- Supportive Care for Rhabdomyolysis
- Aggressive hydration: To prevent renal damage.
- Electrolyte management: To correct imbalances (especially potassium and calcium).
- Treatment of compartment syndrome if present.
- Stopping Offending Drugs: Discontinuing any medications that are suspected to be causing hemolytic anemia.
- Management of Transfusion Reactions: Immediate cessation of the transfusion. Supportive care, including hydration and management of complications.
Supportive Care
- Hydration: Maintaining adequate hydration is crucial to prevent renal damage by diluting the hemoglobin in the urine and promoting its excretion. Intravenous fluids may be necessary in severe cases.
- Electrolyte Management: Monitoring and correcting electrolyte imbalances, especially in rhabdomyolysis and severe hemolysis.
- Blood Transfusions: May be necessary to correct anemia in severe cases.
- Dialysis: In severe cases of acute kidney injury, dialysis may be required to support renal function.
- Monitoring renal function: Regularly monitoring urine output, serum creatinine, and other renal function markers is essential.
Complications of Hemoglobinuria
Hemoglobinuria, if left untreated or if severe, can lead to several serious complications, primarily due to the toxic effects of free hemoglobin on the kidneys and the systemic effects of the underlying hemolytic process.
Acute Renal Failure (Acute Kidney Injury – AKI)
This is the most significant complication.
- Mechanism: Free hemoglobin can precipitate in the renal tubules, forming casts that obstruct urine flow. Additionally, heme, a component of hemoglobin, can cause direct tubular damage through oxidative stress and inflammation.
- Clinical Presentation: Decreased urine output, elevated creatinine and BUN levels, electrolyte imbalances.
- Severity: Can range from mild renal impairment to severe, life-threatening kidney failure requiring dialysis.
Chronic Kidney Disease (CKD)
Repeated episodes of hemoglobinuria or prolonged exposure to free hemoglobin can lead to chronic kidney damage.
- Mechanism: Ongoing tubular damage and inflammation can result in progressive fibrosis and loss of kidney function.
- Clinical Presentation: Gradual decline in renal function, proteinuria, hypertension.
Disseminated Intravascular Coagulation (DIC)
In severe cases of intravascular hemolysis, particularly those associated with infections or transfusion reactions, DIC can occur.
- Mechanism: The release of procoagulant substances from damaged red blood cells can trigger widespread activation of the coagulation cascade, leading to both thrombosis and bleeding.
- Clinical Presentation: Thrombosis, bleeding, organ dysfunction.
Iron Overload
Chronic hemolysis and repeated blood transfusions can lead to iron accumulation in various organs, including the liver, heart, and endocrine glands.
- Mechanism: The body has limited capacity to excrete excess iron, and it can accumulate, causing organ damage.
- Clinical presentation: fatigue, joint pain, abdominal pain, heart problems, and endocrine dysfunction.
Other Complications
- Electrolyte imbalances: Especially in rhabdomyolysis induced hemoglobinuria.
- Infections: Especially in patients with underlying conditions that increase infection risk.
- Cardiovascular complications: In severe anemia.
Prevention of Hemoglobinuria
Prevention of hemoglobinuria depends on the underlying cause.
- Safe Transfusion Practices: Strict adherence to blood typing and crossmatching procedures is essential to prevent ABO incompatibility reactions. Careful monitoring of patients during and after transfusions can help detect delayed hemolytic reactions.
- Avoiding Exposure to Toxins: Educating individuals about the risks of exposure to certain toxins, such as snake venoms or industrial chemicals.
- Genetic Counseling for Inherited Hemolytic Anemias: Providing genetic counseling to individuals with a family history of inherited hemolytic anemias, such as G6PD deficiency or PNH and educating affected individuals about triggers to avoid.
- Appropriate Hydration During Strenuous Exercise: Encouraging adequate hydration during intense physical activity to prevent rhabdomyolysis and march hemoglobinuria.
- Prompt Treatment of Infections: Early diagnosis and treatment of infections, especially malaria and clostridial infections, can prevent severe hemolysis.
- Careful Medication Monitoring: Closely monitoring patients taking medications that can cause hemolytic anemia. Promptly discontinuing any suspected offending drugs.
- Management of Chronic Conditions: Consistent and appropriate management of chronic conditions like autoimmune hemolytic anemia and PNH to minimize hemolytic episodes.
Frequently Asked Questions (FAQs)
What is the difference between hemoglobinuria and myoglobinuria?
Hemoglobinuria and myoglobinuria both result in the presence of protein in the urine, often causing discoloration, but they originate from different sources within the body.
| Feature | Hemoglobinuria | Myoglobinuria |
| Source | Breakdown of red blood cells (intravascular hemolysis) | Breakdown of muscle tissue (rhabdomyolysis) |
| Protein in Urine | Hemoglobin | Myoglobin |
| Causes | Transfusion reactions Hemolytic anemias Severe infections (malaria) Mechanical damage to RBCs | Crush injuries Severe muscle traumaExcessive exercise Certain drug reactions |
| Clinical Significance | Indicates red blood cell destruction within the bloodstream | Indicates muscle tissue damage |
| Urine dipstick for “blood” | Positive | Positive |
| Differentiating test | Further laboratory tests are needed to measure free hemoglobin. | Further laboratory tests are needed to measure myoglobin. |
| Clinical Context | Often there are other signs of haemolysis, such as anemia, or jaundice. | Often there are signs of muscle damage, such as muscle pain, and weakness. |
Can hemoglobinuria cause proteinuria?
Yes, hemoglobinuria can indeed contribute to proteinuria. Here’s how:
- Kidney Damage: As discussed earlier, free hemoglobin can be toxic to the renal tubules. This damage can disrupt the normal filtration processes of the kidneys, allowing proteins to leak into the urine. Specifically, the damage to the glomeruli, the kidney’s filtering units, can lead to increased permeability, resulting in protein passing into the urine.
- Tubular Proteinuria: The renal tubules are responsible for reabsorbing proteins that pass through the glomeruli. Damage to these tubules can impair their reabsorption capacity, leading to increased protein excretion in the urine.
Therefore, while hemoglobinuria’s primary characteristic is the presence of free hemoglobin in the urine, it can also lead to proteinuria as a secondary consequence of kidney damage.
Can a UTI cause hemoglobinuria?
A urinary tract infection (UTI) primarily causes hematuria (the presence of red blood cells in urine), not hemoglobinuria (the presence of free hemoglobin). While a severe UTI, particularly a kidney infection (pyelonephritis), might cause some degree of kidney damage that could theoretically lead to a very small amount of hemoglobin being present, it is not a typical or common cause of clinically significant hemoglobinuria. Therefore, if hemoglobinuria is present, it is more likely due to another underlying condition rather than the UTI itself.
What drugs can cause hemoglobinuria?
Several drugs can potentially cause hemoglobinuria, primarily by inducing hemolytic anemia.
Drugs inducing immune hemolytic anemia
These drugs can trigger the immune system to attack red blood cells. Examples include:
- Cephalosporins (a class of antibiotics)
- Methyldopa
- Penicillins
- Quinidine
- Rifampin
- Sulfonamides
Drugs causing oxidative hemolysis
These drugs can cause red blood cell damage through oxidative stress, especially in individuals with G6PD deficiency. Examples include:
- Dapsone
- Phenazopyridine
Other drugs
There are other drugs that can cause hemolytic anemia through various mechanisms.
- Amphotericin B.
Disclaimer: This article is intended for informational purposes only and is specifically targeted towards medical students. It is not intended to be a substitute for informed professional medical advice, diagnosis, or treatment. While the information presented here is derived from credible medical sources and is believed to be accurate and up-to-date, it is not guaranteed to be complete or error-free. See additional information.
References
- https://www.msdmanuals.com/professional/hematology-and-oncology/anemias-caused-by-hemolysis/autoimmune-hemolytic-anemia
- Phillips J, Henderson AC. Hemolytic Anemia: Evaluation and Differential Diagnosis. Am Fam Physician. 2018 Sep 15;98(6):354-361. PMID: 30215915.
- Mohanty S, Casella M, Compagnucci P, Torlapati PG, Della Rocca DG, La Fazia VM, Gianni C, Chierchia GB, MacDonald B, Mayedo A, Khan UN, Allison J, Bassiouny M, Gallinghouse GJ, Burkhardt JD, Horton R, Al-Ahmad A, Di Biase L, de Asmundis C, Russo AD, Natale A. Acute Kidney Injury Resulting From Hemoglobinuria After Pulsed-Field Ablation in Atrial Fibrillation: Is it Preventable? JACC Clin Electrophysiol. 2024 Apr;10(4):709-715. doi: 10.1016/j.jacep.2023.12.008. Epub 2024 Feb 1. PMID: 38310489.