Key Takeaways
Hematuria is the presence of blood in the urine, either visible (gross) or microscopic.
- Causes ▾: Ranges from benign (UTIs, stones, exercise) to serious (glomerulonephritis, cancer).
- Symptoms ▾: Can be asymptomatic or include pain, frequency, urgency, fever.
- Investigations ▾: Urinalysis, urine culture, blood tests, imaging (ultrasound, CT, cystoscopy).
- Treatment ▾: Addresses the underlying cause (antibiotics, pain management, surgery).
- Complications ▾: Anemia, renal failure, urinary obstruction, infection.
- Prevention ▾: Hydration, managing risk factors, prompt UTI treatment, and regular checkups.
*Click ▾ for more information
Introduction
Hematuria is a medical term that refers to the presence of blood in the urine. Even a small amount of blood can cause a noticeable color change in the urine. It can be categorized into two main types:
- Gross hematuria: This is when the blood in the urine is visible to the naked eye. The urine may appear pink, red, or brown.
- Microscopic hematuria: In this case, the blood is not visible to the naked eye and can only be detected through a urinalysis, which is a laboratory test of the urine.
Hematuria (blood in urine) can be a sign of various underlying conditions, ranging from relatively benign issues like urinary tract infections to more serious problems like kidney disease or cancer.
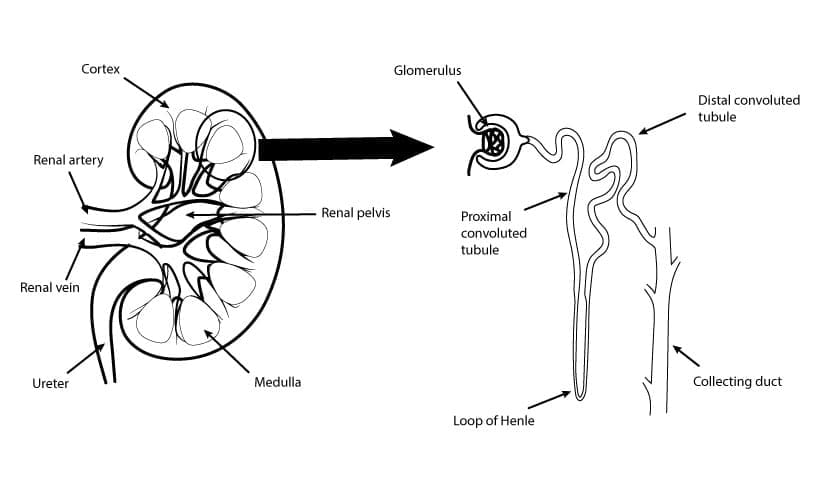
Anatomy of the Urinary Tract

- Kidneys: These are paired organs located in the retroperitoneal space. Their primary function is to filter waste products and excess fluid from the blood to produce urine. Each kidney contains millions of nephrons, the functional units where filtration occurs. Damage or disease within the nephrons (glomeruli, tubules) can lead to blood entering the urine.
- Ureters: These are thin tubes that transport urine from the kidneys to the bladder. Stones, tumors, or infections within the ureters can cause bleeding.
- Bladder: This is a muscular sac that stores urine until it’s eliminated from the body. Infections, stones, tumors, or trauma to the bladder wall can result in blood in the urine.
- Urethra: This is the tube that carries urine from the bladder to the outside of the body. Infections, strictures, or trauma to the urethra can cause bleeding.
- Prostate (in males): The prostate gland surrounds the urethra. Enlargement of the prostate (BPH), prostatitis, or prostate cancer can cause blood in the urine.
Being able to differentiate between kidney, ureter, bladder, prostate, or urethral causes of hematuria (blood in urine), greatly changes the course of treatment.
Causes of Hematuria (Blood in Urine)
The causes of hematuria ranges from benign causes to more complicated and serious ones. All of them should not be ignored and must be medically evaluated.
Glomerular Causes (Kidney’s Filtration Units)
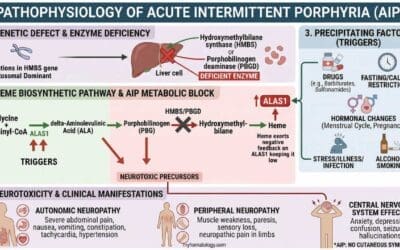
- Glomerulonephritis: This is inflammation of the glomeruli, the tiny filters in the kidneys. These conditions disrupt the filtration process, allowing RBCs to leak into the urine.
- Various types exist, including:
- IgA nephropathy: Often triggered by an upper respiratory infection.
- Post-streptococcal glomerulonephritis: Occurs after a strep infection.
- Lupus nephritis: Associated with systemic lupus erythematosus (SLE).
- Anti-glomerular basement membrane (anti-GBM) disease (Goodpasture’s syndrome).
- Various types exist, including:
- Alport Syndrome: A genetic disorder affecting the glomerular basement membrane. This disorder leads to progressive kidney disease, hearing loss, and eye abnormalities.
- Thin Basement Membrane Disease: A benign condition where the glomerular basement membrane is abnormally thin. It often causes microscopic hematuria (blood in urine).
Tubular and Interstitial Causes (Kidney’s Tubules and Surrounding Tissue)
- Acute Tubular Necrosis (ATN): Damage to the kidney’s tubules, often due to ischemia (lack of blood flow) or toxins. This can lead to hematuria (blood in urine) and impaired kidney function.
- Interstitial Nephritis: Inflammation of the kidney’s interstitial tissue, often caused by medications or infections. It can result in hematuria (blood in urine), fever, and rash.
- Papillary Necrosis: Damage to the renal papillae. This is often associated with sickle cell disease, analgesic abuse, or diabetes.
Urological Causes (Urinary Tract Structures)
- Urinary Tract Infections (UTIs): Infections in any part of the urinary tract (kidneys, ureters, bladder, urethra). Inflammation and irritation can cause bleeding.
- Kidney Stones (Nephrolithiasis) and Bladder Stones (Cystolithiasis): Hard mineral deposits that can cause irritation and bleeding as they move through the urinary tract. This is often associated with severe pain.
- Urethral Strictures: Narrowing of the urethra, often due to scarring from infection or injury. Strictures can cause bleeding and difficulty urinating.
- Benign Prostatic Hyperplasia (BPH) (in men): Enlargement of the prostate gland, which can compress the urethra and cause bleeding.
- Bladder Cancer, Kidney Cancer, and Ureteric Cancer: Malignant tumors in the urinary tract can cause gross or microscopic hematuria (blood in urine).
Traumatic Causes
- Kidney, Bladder, or Urethral Injury: Trauma from accidents or sports injuries can cause significant bleeding.
Other Causes
- Strenuous Exercise: Can cause temporary hematuria (blood in urine).
- Medications: Anticoagulants (e.g., warfarin, heparin) and antiplatelet drugs (e.g. aspirin, clopidogrel) can increase the risk of bleeding.
- Sickle Cell Disease: Can cause kidney damage and hematuria due to vaso-occlusion of blood vessels.
- Coagulation Disorders: Conditions that affect blood clotting can lead to hematuria (blood in urine).
- False Hematuria:
- Red or pink discoloration of urine due to:
- Certain foods (e.g., beets, blackberries).
- Medications (e.g., rifampin).
- Menstrual contamination.
- Myoglobinuria, caused by rhabdomyolysis, can also cause a red colour to the urine.
- Red or pink discoloration of urine due to:
Gender Differences in Hematuria (Blood in Urine)
Specific Causes in Men
When considering hematuria (blood in urine) in men, some causes are more prevalent or unique due to their anatomy and physiology.
Benign Prostatic Hyperplasia (BPH)
This is a very common cause of hematuria (blood in urine) in older men. The prostate gland enlarges with age, compressing the urethra and potentially damaging small blood vessels. This can lead to both gross and microscopic hematuria (blood in urine), often accompanied by other urinary symptoms like:
- Frequency and urgency of urination.
- Weak urine stream.
- Nocturia (frequent urination at night).
It’s crucial to differentiate BPH from prostate cancer, as both can cause hematuria (blood in urine).
Prostate Cancer
Prostate cancer is another significant cause of hematuria (blood in urine) in men, especially in older age groups. While hematuria (blood in urine) may not always be the primary symptom, it can occur as the tumor grows and invades surrounding tissues. Other symptoms may include:
- Difficulty urinating.
- Pain or burning during urination.
- Pain in the lower back, hips, or pelvis.
A PSA (prostate-specific antigen) test and a digital rectal exam are essential for evaluating potential prostate cancer.
Prostatitis
Prostatitis, or inflammation of the prostate gland, can cause hematuria (blood in urine), along with:
- Pelvic pain.
- Painful ejaculation.
- Dysuria (painful urination).
- This can be caused by bacterial infections, or other inflammatory processes.
This is more common in younger to middle aged men.
Urethral Strictures
Narrowing of the urethra, often due to past infections, trauma, or instrumentation. Strictures can cause hematuria (blood in urine), pain during urination, and a weak urine stream.
Urinary Tract Infections (UTIs)
While UTIs are more common in women, they can still occur in men and cause hematuria. Risk factors in men include:
- BPH.
- Uncircumcised penis.
- Instrumentation of the urinary tract.
Kidney Stones
Kidney stones can cause significant pain and hematuria as they pass through the ureters. Men are more prone to kidney stones than women.
Specific Causes in Women
When discussing hematuria in women, it’s essential to consider causes that are more prevalent or unique to their physiology.
Urinary Tract Infections (UTIs)
UTIs are significantly more common in women due to their shorter urethra, which allows bacteria easier access to the bladder. Cystitis (bladder infection) and pyelonephritis (kidney infection) can both cause hematuria (blood in urine), along with other symptoms like:
- Dysuria (painful urination).
- Frequency and urgency of urination.
- Pelvic pain.
- Fever and chills (especially in pyelonephritis).
Menstrual Contamination
This is a common cause of “false hematuria” in women. Blood from menstruation can mix with urine, leading to a red or pink discoloration. It’s crucial to differentiate menstrual contamination from true hematuria. Proper urine collection techniques (midstream clean-catch) can help minimize this issue.
Urethral Diverticulum
This is a small pouch or outpouching in the urethra. It can become infected or irritated, leading to hematuria (blood in urine), pain, and other urinary symptoms.
Interstitial Cystitis/Bladder Pain Syndrome (IC/BPS)
While not always causing visible hematuria, IC/BPS is a chronic condition that can cause microscopic hematuria (blood in urine), along with:
- Pelvic pain.
- Urinary urgency and frequency.
Kidney Stones
While kidney stones affect both men and women, they can cause significant blood in the urine and pain in women.
Glomerulonephritis
- Kidney related glomerular diseases, such as IgA nephropathy, Lupus nephritis and other forms of glomerulonephritis, can affect women and cause blood in the urine.
Urological cancers
Bladder, kidney and ureteric cancers can occur in women and causing blood in the urin.
Signs and Symptoms Associated with Hematuria
Gross Hematuria (Visible Blood in Urine)
- Appearance: The urine may appear pink, red, or brown. The intensity of the color depends on the amount of blood present. Clots may be visible in the urine, which can indicate more significant bleeding.
- Associated Symptoms:
- May be asymptomatic (no other symptoms).
- Pain: Flank pain (kidney stones, pyelonephritis), suprapubic pain (bladder infection), or dysuria (painful urination).
- Urinary urgency and frequency.
- Fever and chills (infection).
- Symptoms of systemic disease (edema, hypertension).
Microscopic Hematuria (Blood Detectable Only by Urinalysis)
- Appearance: The urine appears normal to the naked eye.
- Associated Symptoms: Often asymptomatic. If symptoms are present, they are related to the underlying cause (e.g., symptoms of glomerulonephritis, kidney stones, or infection).
Symptoms Related to Underlying Causes
- Urinary Tract Infections (UTIs)
- Dysuria (painful urination).
- Urinary frequency and urgency.
- Pelvic pain.
- Fever and chills (pyelonephritis).
- Kidney Stones
- Severe flank pain (renal colic).
- Pain radiating to the groin.
- Nausea and vomiting.
- Glomerulonephritis
- Edema (swelling), particularly in the legs and around the eyes.
- Hypertension.
- Fatigue.
- Bladder or Kidney Cancer
- May be asymptomatic, especially in early stages.
- Painful urination.
- Pelvic pain.
- Unexplained weight loss.
- Benign Prostatic Hyperplasia (BPH)
- Weak urine stream.
- Difficulty starting urination.
- Nocturia (frequent urination at night).
- Urinary frequency and urgency.
- Trauma
- Pain in the flank, abdomen, or pelvis.
- Bruising.
- Systemic Diseases
- Symptoms related to the underlying disease (e.g., rash in lupus, joint pain in vasculitis).
Laboratory Investigations of Hematuria
Laboratory investigations are crucial for determining the cause and severity of blood in urine
Urinalysis
- Dipstick Testing: This is a quick screening test that detects the presence of blood (hemoglobin) in the urine. It can also detect other abnormalities like protein, glucose, leukocytes (white blood cells), and nitrites, which can provide clues to the underlying cause.
- Microscopic Examination: This involves examining a urine sample under a microscope to count the number of red blood cells (RBCs). It can also identify other cells, such as white blood cells (WBCs), epithelial cells, and casts. The presence of RBC casts is particularly significant, as it suggests glomerular bleeding.
- Urine Cytology: This is a test that examines urine cells for abnormalities. It is used to detect cancer cells in the urinary tract.
Urine Culture
This test is performed to identify bacterial infections in the urinary tract. It’s essential if a UTI is suspected, as it helps determine the specific bacteria causing the infection and guide antibiotic therapy.
Blood Tests
- Complete Blood Count (CBC): This test assesses red blood cell count, white blood cell count, and platelet count. It can detect anemia (low red blood cell count) due to chronic bleeding or infection (high white blood cell count).
- Renal Function Tests: These tests measure blood urea nitrogen (BUN) and creatinine levels to evaluate kidney function. They are essential for detecting kidney disease or damage. eGFR (estimated glomerular filtration rate) is also calculated to assess kidney function.
- Coagulation Studies: These tests assess blood clotting ability. They are performed if a bleeding disorder is suspected.
- Prostate-Specific Antigen (PSA) Test (in men): This test measures PSA levels in the blood, which can be elevated in prostate cancer or BPH. This test is very important in men with hematuria.
- Complement levels: These can be useful when glomerulonephritis is suspected.
- Antinuclear antibodies (ANA) and anti-neutrophil cytoplasmic antibodies (ANCA): These tests can be used when autoimmune causes of glomerulonephritis are suspected.
- Sickle cell testing: If sickle cell disease is suspected.
Imaging Studies (Often Considered After Initial Lab Tests)
- Ultrasound of the Kidneys and Bladder: This is a non-invasive imaging technique that can visualize the kidneys, ureters, and bladder. It can detect kidney stones, tumors, and other abnormalities.
- CT Scan (with or without contrast): This imaging technique provides detailed images of the urinary tract. It can detect kidney stones, tumors, and other structural abnormalities.
- Cystoscopy: This is an invasive procedure that involves inserting a thin, flexible tube with a camera into the bladder. It allows direct visualization of the bladder and urethra and can detect tumors, stones, and other abnormalities.
- Intravenous Pyelogram (IVP): Though less common now, due to CT scans, this is an X-ray examination of the kidneys, ureters, and bladder that uses a contrast dye injected into a vein.
- Renal Biopsy: In cases of suspected glomerular disease, a renal biopsy may be needed to obtain a tissue sample for microscopic examination.
General Treatment and Management of Hematuria
The treatment and management of blood in urinedepend entirely on the underlying cause.
Addressing the Underlying Cause
Urinary Tract Infections (UTIs)
Antibiotics are the mainstay of treatment. The specific antibiotic and duration of treatment depend on the type of bacteria causing the infection.
Kidney Stones
- Pain management: NSAIDs or opioids for pain relief.
- Increased fluid intake to help pass the stone.
- Alpha-blockers: Medications to relax the ureter and facilitate stone passage.
- Lithotripsy: Shock wave therapy to break up large stones.
- Ureteroscopy or percutaneous nephrolithotomy: Surgical procedures for larger or impacted stones.
Glomerulonephritis
Treatment depends on the specific type of glomerulonephritis. Corticosteroids and immunosuppressants may be used to reduce inflammation. Blood pressure control is essential and dietary modifications may be necessary.
Bladder or Kidney Cancer
- Surgery: To remove the tumor.
- Chemotherapy: To kill cancer cells.
- Radiation therapy: To shrink the tumor.
- Immunotherapy: To boost the immune system’s ability to fight cancer.
Benign Prostatic Hyperplasia (BPH)
- Alpha-blockers: To relax the prostate and improve urine flow.
- 5-alpha-reductase inhibitors: To shrink the prostate.
- Minimally invasive procedures or surgery: For severe cases.
Trauma
Treatment depends on the extent of the injury. Rest and observation for minor injuries while surgery is an option for severe injuries.
Medication-induced hematuria
Adjustment or discontinuation of the causative medication, when possible, under medical supervision.
Coagulation disorders
Treatment of the underlying disorder and medications to correct coagulation abnormalities.
Supportive Care
- Hydration: Increased fluid intake can help flush out the urinary tract and prevent complications.
- Pain Control: Pain relievers can be used to manage discomfort.
- Monitoring: Regular monitoring of urine output and kidney function is essential.
Referral to Specialists
- Nephrology: For kidney-related causes.
- Urology: For urological causes, such as kidney stones, tumors, or BPH.
- Oncology: For cancer-related causes.
Follow-up
Follow-up urinalysis and other tests may be necessary to ensure that the blood in urine has resolved and that the underlying condition is being managed effectively. Regular checkups are crucial, particularly for chronic conditions or malignancies.
Complications of Hematuria
Hematuria, while a symptom itself, can lead to various complications depending on the underlying cause and the severity of the bleeding.
- Anemia: Chronic or heavy blood loss in the urine can lead to iron deficiency anemia. This results in a decreased number of red blood cells, causing fatigue, weakness, and pallor.
- Renal Failure: If the blood in the urine is caused by kidney disease (e.g., glomerulonephritis) or urinary tract obstruction, it can lead to impaired kidney function and, in severe cases, renal failure. Obstruction can cause back pressure on the kidneys, which damages them. Glomerular diseases directly damage the filtering units of the kidney.
- Urinary Tract Obstruction: Blood clots in the urine can obstruct the flow of urine, leading to:
- Pain.
- Difficulty urinating.
- Urinary retention.
This is especially dangerous if it obstructs both kidneys, or a single functioning kidney.
- Infection: Hematuria caused by a UTI can lead to more severe infections, such as pyelonephritis (kidney infection) or sepsis (blood infection). The presence of blood can also increase the risk of secondary infections.
- Progression of Underlying Disease: If the blood in the urine is a symptom of a serious condition like cancer, delayed diagnosis and treatment can lead to disease progression and metastasis. Untreated glomerulonephritis can lead to end stage renal disease.
- Psychological Distress: The sight of blood in the urine can be alarming and cause significant anxiety and stress. Chronic hematuria can also affect quality of life.
- Complications from treatment: Some treatments, such as surgery, or radiation therapy, can have their own complications.
Prevention of Hematuria
Preventing blood in the urine largely depends on addressing the underlying risk factors and maintaining good urinary tract health.
Lifestyle Modifications
- Hydration:Drinking plenty of water helps dilute urine and flush out irritants, reducing the risk of urinary tract infections and kidney stones.
- Dietary Changes:For individuals prone to kidney stones, dietary modifications may be necessary. This might include:
- Limiting sodium intake.
- Adjusting calcium intake (as advised by a doctor).
- Reducing oxalate-rich foods (e.g., spinach, rhubarb).
- Limiting animal protein.
- Maintaining a Healthy Weight: Obesity can increase the risk of kidney stones and other urinary tract problems.
Management of Risk Factors
- Prompt Treatment of UTIs: Seeking prompt medical attention for symptoms of a UTI can prevent the infection from spreading to the kidneys and causing hematuria.
- Control of Chronic Diseases: Managing conditions like diabetes and hypertension can help prevent kidney damage and hematuria.
- Medication Management: Discussing medications with a doctor, especially anticoagulants and antiplatelet drugs, can help minimize the risk of bleeding.
- Avoiding Irritants: Avoiding irritants to the bladder, such as certain foods or chemicals, can help prevent hematuria.
- Safe Sexual Practices: To reduce the risk of UTIs.
Regular Medical Checkups
- Screening for Prostate Cancer (in men): Regular PSA testing and digital rectal exams can help detect prostate cancer early, when it’s more treatable.
- Regular Kidney Function Tests: For people with chronic diseases, or a family history of kidney disease.
- Yearly general checkups: To catch any possible issues early.
Injury Prevention
- Protective Gear: Wearing appropriate protective gear during sports or other activities can help prevent traumatic injuries to the kidneys and bladder.
- Safe driving habits: To limit the risk of car accidents.
Hygiene Practices
Practicing good hygiene, especially after sexual activity, can help prevent UTIs. Women should wipe from front to back after using the toilet.
Frequently Asked Questions (FAQs)
What are red flags for hematuria?
Red flags in hematuria are signs and symptoms that suggest a potentially serious underlying condition requiring urgent evaluation. These warrant prompt medical attention.
- Gross Hematuria (Visible Blood in Urine): Any visible blood in the urine, regardless of other symptoms. Especially if accompanied by blood clots.
- Pain
- Severe flank pain (renal colic) radiating to the groin: Suggests kidney stones.
- Persistent pelvic pain: May indicate bladder cancer or other serious conditions.
- Pain during urination (dysuria) along with hematuria: Could be a sign of severe infection or other serious issues.
- Associated Symptoms
- Unexplained weight loss.
- Fever and chills: Suggests a serious infection, such as pyelonephritis or an abscess.
- Edema (swelling) in the legs or around the eyes: May indicate kidney disease.
- Hypertension (high blood pressure).
- Difficulty urinating or urinary retention.
- Symptoms of systemic illness (e.g., fatigue, night sweats).
- Risk Factors
- Age over 40-50: Increased risk of bladder or kidney cancer.
- Smoking history: Significantly increases the risk of bladder cancer.
- Occupational exposure to certain chemicals (e.g., dyes, solvents).
- History of pelvic radiation.
- History of chronic urinary tract infections.
- Family history of kidney disease or urinary tract cancers.
- History of kidney stones.
- History of gross hematuria, even if resolved.
- Laboratory Findings
- Elevated creatinine or BUN levels: Indicates impaired kidney function.
- Presence of red blood cell casts in the urine: Suggests glomerular disease.
- Elevated PSA in men: Raises suspicion for prostate cancer.
- Circumstances of onset: Hematuria following trauma, especially blunt trauma to the flank or abdomen.
Why Are These Red Flags?
These symptoms can indicate serious conditions like:
- Cancer (bladder, kidney, prostate).
- Severe kidney disease (glomerulonephritis).
- Severe infections (pyelonephritis, abscess).
- Significant trauma.
- Urinary tract obstructions.
Prompt evaluation is essential to:
- Identify the underlying cause.
- Initiate timely treatment.
- Prevent complications.
How much blood in urine is considered hematuria?
Hematuria is defined as the presence of red blood cells (RBCs) in the urine. While gross hematuria refers to visible blood, even a microscopic amount is clinically significant. Specifically, microscopic hematuria is generally defined as 3 or more RBCs per high-power field on a microscopic urinalysis. Therefore, any amount of blood detected through a urine test is considered hematuria, and a medical evaluation is warranted.
What is mistaken for hematuria?
Several conditions and substances can cause urine discoloration that may be mistaken for hematuria.
- Foods: Beets, blackberries, and rhubarb can cause a reddish or pinkish discoloration of urine.
- Medications: Rifampin (an antibiotic), phenazopyridine (a urinary analgesic), and some laxatives can alter urine color.
- Myoglobinuria: This is the presence of myoglobin (a muscle protein) in the urine, often caused by rhabdomyolysis (muscle breakdown). It can cause a reddish-brown discoloration.
- Porphyria: A rare genetic disorder that can cause reddish-brown urine.
- Menstrual Contamination: In women, menstrual blood can mix with urine, leading to a false appearance of hematuria.
- Concentrated Urine: Very concentrated urine can appear darker, and sometimes reddish.
- Certain dyes: Some dyes used in food or medications can give urine a reddish hue.
- Urates: Especially in newborns, urate crystals can make the urine appear pink.
Can hematuria resolve itself?
Yes, hematuria can sometimes resolve itself, especially in cases where the underlying cause is transient or mild. However, it’s crucial to understand that even if it resolves, a medical evaluation is still necessary to determine the cause. Hematuria due to serious causes like kidney stones, glomerulonephritis, bladder or kidney cancer needs proper treatment.
Transient Causes
- Strenuous exercise: Hematuria caused by intense physical activity often resolves on its own within a few days.
- Mild urinary tract infections (UTIs): In some cases, mild UTIs may resolve spontaneously, but this is not recommended, and antibiotics are usually necessary.
- Minor trauma: Small injuries to the urinary tract may heal without intervention.
- Medication or food related: Once the offending agent is removed, the hematuria will resolve.
Can stress cause blood in urine?
While stress itself doesn’t directly cause blood in the urine (hematuria), it can exacerbate or contribute to conditions that do. For instance, stress can worsen interstitial cystitis, which may lead to microscopic hematuria and bladder pain. Additionally, stress can weaken the immune system, potentially increasing susceptibility to urinary tract infections, which can cause hematuria. However, isolated stress is not considered a primary cause of hematuria, and any instance of blood in urine necessitates medical evaluation to rule out serious underlying conditions.
Is peeing blood an emergency?
Peeing blood, or gross hematuria, can indicate a serious underlying condition and should be considered an urgent medical concern, though not always a life-threatening emergency. While some causes may be relatively benign, others, like kidney stones causing severe obstruction, or bladder cancer, require prompt evaluation and treatment. Therefore, immediate medical attention is necessary to determine the cause and prevent potential complications.
How much blood in urine is worrying?
Any visible blood in the urine (gross hematuria) is concerning and warrants medical evaluation. Even microscopic hematuria, detected only by urinalysis, requires investigation. While the amount of blood doesn’t necessarily correlate with the severity of the underlying condition, the presence of any blood indicates a potential problem that needs to be addressed to rule out serious causes like infections, kidney stones, or cancer.
Why am I peeing blood but no pain?
Painless hematuria can be concerning because it may indicate serious underlying conditions, such as bladder or kidney cancer, which often present without pain in their early stages. Other potential causes include certain types of glomerulonephritis, benign prostatic hyperplasia (BPH) in men, or even certain medications. While less common, some kidney stones or infections can also cause painless hematuria. Therefore, even without pain, any instance of blood in urine requires prompt medical evaluation to determine the cause and initiate appropriate treatment.
Disclaimer: This article is intended for informational purposes only and is specifically targeted towards medical students. It is not intended to be a substitute for informed professional medical advice, diagnosis, or treatment. While the information presented here is derived from credible medical sources and is believed to be accurate and up-to-date, it is not guaranteed to be complete or error-free. See additional information.
References
- Linder BJ, Bass EJ, Mostafid H, Boorjian SA. Guideline of guidelines: asymptomatic microscopic haematuria. BJU Int. 2018 Feb;121(2):176-183. doi: 10.1111/bju.14016. Epub 2017 Nov 2. PMID: 28921833.
- Sountoulides P, Mykoniatis I, Metaxa L. Non-visible asymptomatic haematuria: a review of the guidelines from the urologist’s perspective. Expert Rev Anticancer Ther. 2017 Mar;17(3):203-216. doi: 10.1080/14737140.2017.1284589. Epub 2017 Jan 27. PMID: 28116915.
- Mears A, Colemeadow J, Johal NS. Haematuria in children. Br J Hosp Med (Lond). 2021 May 2;82(5):1-8. doi: 10.12968/hmed.2021.0046. Epub 2021 May 26. PMID: 34076519.