Procedure-at-a-Glance
The ESR is a simple, inexpensive blood test that measures how quickly red blood cells settle in a vertical tube over one hour, expressed in millimeters per hour (mm/hr). It is a non-specific marker of inflammation [6].
- Collect venous blood using the appropriate tube.
- Gently invert the tube 8 - 10 times.
- Fill the Westergren tube to the '0' mark and place it in the rack.
- Leave the tube undisturbed at room temperature (20-25°C) for exactly 60 minutes. For some semi-automated or automated machines, readings can be taken at 30 minutes.
- Measure the height of the clear plasma from the top (0) to the top of the red cell column.
Why ESR Still Matters
Faster, more sensitive markers like CRP exist. So why is ESR still ordered every day in hospitals around the world? Because it is cheap, requires no expensive reagents, and remains genuinely useful for monitoring chronic inflammatory disease over weeks and months. For conditions like giant cell arteritis and polymyalgia rheumatica, ESR is part of the diagnostic criteria themselves [5].
This article walks through the principle, the protocol, and the pitfalls of interpretation.
Introduction
The erythrocyte sedimentation rate (ESR), sometimes called the sed rate or Westergren test, measures the rate at which red blood cells (RBCs) settle to the bottom of a vertical tube over one hour. Fahraeus first described the phenomenon in 1918, and Westergren refined the method in 1920. The Westergren tube still bears his name [6].
Because the manual technique involves filling an open glass pipette with whole blood, biohazard exposure has long been a concern. Modern semi-automated and fully automated analyzers reduce that risk by using closed sampling systems and standard EDTA tubes [1].
ESR vs. CRP
Both ESR and CRP are inflammation markers, but they behave differently in the lab and in the body.
ESR does not measure a single protein. It measures how fast red cells fall, which is influenced indirectly by "sticky" plasma proteins (mainly fibrinogen). Because the result depends on the physical properties of the red cells themselves, ESR can be misled by red cell disorders such as anemia, sickle cell disease, or polycythemia.
ESR is slow. It takes days to rise and can stay elevated for weeks after a patient has recovered. Think of it as a historical record of recent inflammation [6].
CRP is a specific protein produced by the liver in response to cytokines (mainly IL-6) released during injury or infection. It rises within 4–6 hours, peaks at 36–48 hours, and falls quickly once inflammation resolves (half-life around 19 hours). Think of it as a live feed.
For acute infections such as pneumonia or sepsis, CRP is usually preferred. For chronic conditions like temporal arteritis, polymyalgia rheumatica, sometimes systemic lupus erythematosus, ESR remains very useful, particularly because CRP can occasionally be normal during a flare [5,6].
Comparison Table: ESR vs. CRP
| Feature | ESR (Modern Automated) | CRP |
|---|---|---|
| What it measures | Rate of RBC sedimentation / aggregationIndirect marker | Liver-produced acute-phase proteinDirect marker |
| Lab turnaround time | Under 3 minCapillary photometry [7] | 30–60 min |
| Response time | SlowRises after 24–48 hours | FastRises within 4–6 hours |
| Recovery time | SlowWeeks to normalize | FastDays to normalize |
| Sensitivity | LowerCan be normal in early inflammation | HigherDetects minor inflammation |
| Specificity | LowAffected by age, sex, RBC shape | HigherLess affected by non-inflammatory factors |
| Effect of anemia | SignificantFalsely raises ESR | Minimal |
| Effect of age / sex | SignificantRises with age; higher in women | Minimal |
| Best used for | Chronic inflammationGCA, PMR, SLE, Hodgkin's | Acute infectionPost-surgery, sepsis, RA flares [8] |
| Technical errors | Low riskAutomated assay | Low riskAutomated assay |
Principle of ESR
The ESR depends on the difference in density between red cells and plasma. RBCs are denser, so when blood sits undisturbed, they settle to the bottom and clear plasma collects on top.
In health, RBCs repel each other because of their negative surface charge (the zeta potential) so they sediment slowly. During inflammation, the liver releases acute-phase proteins, especially fibrinogen. These proteins neutralize the zeta potential and act as a kind of glue, allowing red cells to stack into elongated columns called rouleaux [6]. Stacked cells fall faster than individual cells, and the ESR rises.
A high ESR therefore points toward inflammation, infection, autoimmune disease, malignancy, or pregnancy, but cannot say which. It must be read alongside the clinical picture and other tests.
The Three Stages of Sedimentation
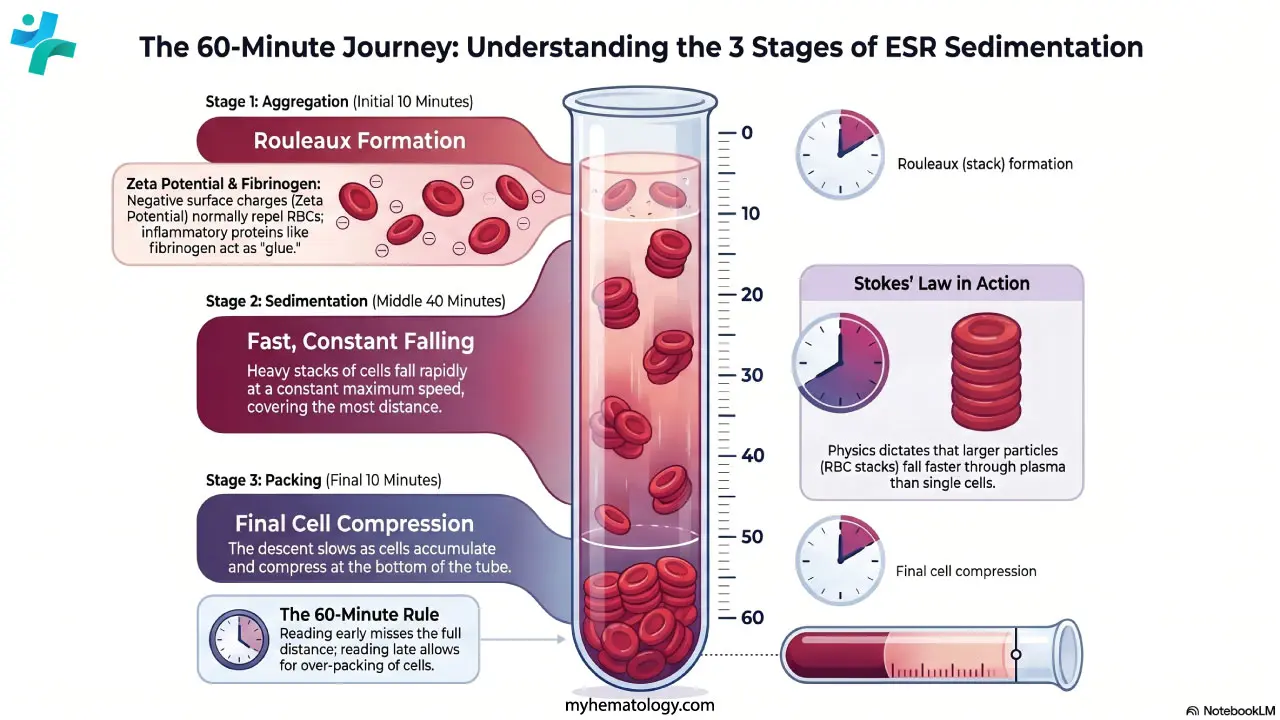
Initial phase — aggregation (≈10 minutes). Individual red cells orient themselves and stack into rouleaux. The more inflammatory protein in the plasma, the more efficient the stacking. If rouleaux formation is blocked for example by sickle cells or spherocytes, the ESR will be falsely low.
Fast phase — sedimentation (≈40 minutes). The heavy stacks fall through the plasma at a roughly constant speed, following Stokes' law: larger particles fall faster than smaller ones through a viscous fluid. Most of the measured distance is covered here. A tilted tube allows cells to slide down the lower wall of the glass, which can substantially elevate the result [3].
Final phase — packing (≈10 minutes). The stacks reach the bottom and compress. Sedimentation slows because the column is now crowded. By the end, plasma and red cells form two clearly separated layers ready to be read.
Why the 60-Minute Rule Matters
Because the three stages take time to complete, the manual ESR is read at exactly 60 minutes. Reading too early (during the fast phase) underestimates the result. Modern automated analyzers can produce a result in 20–30 minutes, but they do this through validated algorithms that extrapolate to a Westergren-equivalent value, not by simply reading the column early [1].
Materials
- EDTA tube (lavender top) for modern automated ESR systems, or 3.8% sodium citrate tube for manual Westergren.
- Sediplast or equivalent system (manual method): pierceable stopper and graduated Westergren tube.
- Vertical rack with a level base.
- Timer.
- Personal protective equipment.
Protocol
Method differs slightly according to the manufacturer's protocol.
- Collect venous blood into the appropriate tube. For the manual method, fill the Sediplast tube with EDTA blood up to the graduation mark and close it with the pierceable stopper (4:1 ratio of blood to citrate diluent in the chamber). For the pure ICSH reference method, undiluted EDTA blood is used in an ICSH-specification Westergren pipette [1,2].
- Mix by gently inverting the tube 8–10 times.
- Set up by inserting the Westergren pipette through the pierceable stopper until it touches the bottom. Capillary action fills the pipette to the zero mark.
- Incubate the tube vertically in the rack at room temperature (20–25°C), away from vibration, draughts, and direct sunlight, for exactly 60 minutes.
- Read the height of the clear plasma column from the zero mark down to the top of the red cell column. Report in mm/hr.
Automated systems
Automated ESR analyzers (for example, Alifax, Test 1, StaRRsed Auto-Compact) read EDTA samples directly using optical or photometric detection. While older automated systems produce a Westergren-equivalent result in 20–30 minutes [1], modern high-throughput laboratories increasingly utilize capillary photometry and automated rheology. These systems measure red blood cell aggregation kinetics using lasers and optical sensors in as little as 20 seconds, mathematically extrapolating a Westergren-equivalent result while eliminating the biohazard risks of open pipettes [8].
Sample stability and quality control
EDTA samples should ideally be analyzed within 4 hours at room temperature or within 24 hours if refrigerated and warmed before testing. If blood sits for longer, red cells become spherical (echinocytes) and lose their ability to stack, falsely lowering the ESR [6].
Interpretation of Erythrocyte Sedimentation Rate (ESR)

Reference Ranges
ESR varies with age and sex. The values below are typical adult ranges; individual laboratories should validate their own.
Age Group |
Male |
Female |
|---|---|---|
| Newborn | 0–2 mm/hr | 0–2 mm/hr |
| Children (up to puberty) | 3–13 mm/hr | 3–13 mm/hr |
| Adults under 50 | 0–15 mm/hr | 0–20 mm/hr |
| Adults 50 and over | 0–20 mm/hr | 0–30 mm/hr |
For older adults, the Miller formula is widely used to set an age-adjusted upper limit [4]:
- Men: age in years ÷ 2
- Women: (age in years + 10) ÷ 2
So for a 70-year-old man the upper limit is 35 mm/hr, and for a 70-year-old woman it is 40 mm/hr. This matters in clinical practice. About a quarter of older patients with confirmed inflammatory or malignant disease still have ESR within the standard reference range, and roughly 6% of patients with polymyalgia rheumatica have a normal ESR at diagnosis [4,6]. A normal result does not rule out disease.
When ESR Is Ordered
ESR is most informative in a small number of clinical situations:
- Evaluating suspected giant cell arteritis, polymyalgia rheumatica, and Hodgkin's lymphoma, where ESR's diagnostic value remains irreplaceable.
- Historically used for monitoring disease activity in rheumatoid arthritis (RA). However, modern rheumatology guidelines increasingly favor CRP over ESR for RA, as CRP correlates significantly better with acute joint inflammation and radiographic progression [9].
- Monitoring disease activity in systemic lupus erythematosus (SLE).
- Working up unexplained constitutional symptoms (fever, weight loss, fatigue) when the cause is unclear.
- Following up known chronic infections such as osteomyelitis or tuberculosis.
Under the 2022 ACR/EULAR classification criteria for giant cell arteritis, an ESR ≥50 mm/hr or CRP ≥10 mg/L contributes 3 points toward the classification score; a total of 6 or more is required [5].
Falsely Elevated ESR
In these situations, red cells fall faster than expected for non-inflammatory reasons.
- Anemia (low hematocrit). The most common cause. Fewer red cells means less crowding, and stacks have a clear path to the bottom.
- Macrocytosis. Larger red cells, as in vitamin B12 or folate deficiency, sediment faster because Stokes' law makes velocity scale with the square of cell radius.
- Pregnancy. From around 10–12 weeks, fibrinogen rises physiologically to prepare for childbirth. ESR can rise substantially. This is a true, expected change, not a laboratory error.
- Renal failure. End-stage kidney disease often produces ESRs above 100 mm/hr because of chronic anemia and altered plasma proteins.
- Tilted tube. Even small deviations from vertical allow cells to slide down the lower wall, bypassing the resistance of plasma rising on the higher side [3].
Falsely Low ESR
These factors can mask serious infection or an autoimmune flare.
- Polycythemia. A high red cell count makes blood thick and crowded. Cells physically cannot fall.
- Abnormal RBC shapes. Rouleaux only form on flat, disc-shaped cells. Sickle cells, spherocytes (seen in hereditary spherocytosis), and acanthocytes all interfere with stacking.
- Hyperviscosity. In conditions like Waldenström's macroglobulinemia, plasma becomes so thick that cells barely move.
- Extreme leukocytosis. A very high white cell count, as in leukemia, physically obstructs the falling red cells.
- Drugs. Corticosteroids, NSAIDs, statins, and oral contraceptives can lower ESR. Always check the medication list before interpreting a borderline result.
- Stale sample. Blood older than 4 hours at room temperature develops echinocytes that do not stack [6].
ESR Clinical Correlation
| Factor | Effect on ESR | Reason |
|---|---|---|
| Anemia | Falsely High | Less crowding, less resistance |
| Tilted Tube | Falsely High | Cells slide down the wall |
| Pregnancy | High (Physiological) | Natural rise in fibrinogen |
| Sickle Cell | Falsely Low | No rouleaux possible |
| Polycythemia | Falsely Low | High blood viscosity |
| Old Sample | Falsely Low | Cells become spherical |
| Cold Temperature | Falsely Low | Plasma viscosity rises |
Modern Methods and Standardization
The Westergren method is still the international reference, reaffirmed by the ICSH and CLSI in 2011 and again in 2017 [1,2]. In practice, however, most laboratories no longer perform it manually. A 2017 ICSH survey of more than 6,000 laboratories found that only 28% of laboratories used the unmodified Westergren method, while 72% used modified or alternate methods, with results sometimes differing from the reference by up to 142% [1]. Each laboratory must therefore validate its analyzer against the Westergren reference and report ESR in Westergren-equivalent units.
FAQs (Frequently Asked Questions)
Why is the ESR test called a "non-specific" test?
ESR confirms inflammation is present somewhere but cannot identify the cause or location. A high ESR can reflect infection, autoimmune disease, cancer, pregnancy, or normal aging. Doctors interpret it alongside symptoms, examination findings, and other tests.
Do I need to fast before an ESR blood test?
No. ESR does not require fasting. Tell your doctor about any medications, because corticosteroids, NSAIDs, statins, and some others can lower the result.
Why do women and older adults have higher "normal" ESR ranges?
ESR rises naturally with age and is generally higher in women than in men of the same age. The Miller formula sets the upper limit of normal as age÷2 in men and (age+10)÷2 in women. A healthy 70-year-old woman can therefore have an ESR up to 40 mm/hr.
Can a normal ESR result mean I am healthy?
Not always. Around 6% of people with polymyalgia rheumatica have a normal ESR at diagnosis, and roughly a quarter of older patients with confirmed inflammatory or malignant disease have ESR within the reference range. Symptoms still matter.
What does a very high ESR mean?
An ESR above 100 mm/hr is unusual and points to a small group of causes: serious infection, certain cancers (especially multiple myeloma and lymphoma), giant cell arteritis, severe kidney disease, or marked anemia. It always warrants further investigation.
How quickly does ESR change with treatment?
ESR moves slowly. It can take days to rise and weeks to fall back to normal even after the cause has resolved. CRP changes within hours, so the two are often ordered together with CRP for the early picture and ESR for the slower trend.
Glossary of Related Medical Terms
- Acute-phase reactant — a plasma protein whose level rises (or falls) sharply during inflammation. Fibrinogen and CRP are common examples.
- Anisocytosis — variation in red cell size on a blood film, which can affect sedimentation.
- Echinocyte — a red cell with short, regular projections, typical of old or stored blood. Echinocytes do not stack well, so ESR falls.
- EDTA — ethylenediaminetetraacetic acid, the standard anticoagulant for full blood counts and modern automated ESR.
- Fibrinogen — a large clotting protein that also acts as glue between red cells, encouraging rouleaux formation.
- Giant cell arteritis (GCA) — inflammation of medium and large arteries in adults over 50, in which ESR is one of the supporting diagnostic criteria.
- Hyperviscosity — abnormally thick plasma, usually from very high protein levels, which paradoxically slows ESR.
- Polymyalgia rheumatica (PMR) — an inflammatory shoulder- and hip-girdle pain syndrome in older adults, often associated with a raised ESR.
- Rouleaux formation — red cells stacking like coins. The faster they stack, the faster the ESR.
- Stokes' law — the rule that larger, denser particles fall faster through a fluid.
- Westergren method — the ICSH reference method for ESR, using a 200 mm vertical pipette read at 60 minutes.
- Zeta potential — the natural negative charge on red cells that keeps them apart in plasma.
Disclaimer: This protocol is for educational purposes only. Local laboratory standard operating procedures take precedence. It is not intended to be a substitute for informed professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare professional for clinical decision-making. While the information presented here is derived from credible medical sources and is believed to be accurate and up-to-date, it is not guaranteed to be complete or error-free. See additional information.
References
- Kratz, A., Plebani, M., Peng, M., Lee, Y. K., McCafferty, R., Machin, S. J., & International Council for Standardization in Haematology (ICSH) (2017). ICSH recommendations for modified and alternate methods measuring the erythrocyte sedimentation rate. International journal of laboratory hematology, 39(5), 448–457. https://doi.org/10.1111/ijlh.12693
- ICSH recommendations for measurement of erythrocyte sedimentation rate. International Council for Standardization in Haematology (Expert Panel on Blood Rheology). (1993). Journal of clinical pathology, 46(3), 198–203. https://doi.org/10.1136/jcp.46.3.198
- Jou, J. M., Lewis, S. M., Briggs, C., Lee, S. H., De La Salle, B., McFadden, S., & International Council for Standardization in Haematology (2011). ICSH review of the measurement of the erythocyte sedimentation rate. International journal of laboratory hematology, 33(2), 125–132. https://doi.org/10.1111/j.1751-553X.2011.01302.x
- Miller, A., Green, M., & Robinson, D. (1983). Simple rule for calculating normal erythrocyte sedimentation rate. British medical journal (Clinical research ed.), 286(6361), 266. https://doi.org/10.1136/bmj.286.6361.266
- Ponte, C., Grayson, P. C., Robson, J. C., Suppiah, R., Gribbons, K. B., Judge, A., Craven, A., Khalid, S., Hutchings, A., Watts, R. A., Merkel, P. A., Luqmani, R. A., & DCVAS Study Group (2022). 2022 American College of Rheumatology/EULAR Classification Criteria for Giant Cell Arteritis. Arthritis & rheumatology (Hoboken, N.J.), 74(12), 1881–1889. https://doi.org/10.1002/art.42325
- Tishkowski K, Zubair M. Erythrocyte Sedimentation Rate. [Updated 2025 Jul 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK557485/
- Bain BJ, Bates I, Laffan MA. Dacie and Lewis Practical Haematology: Expert Consult: Online and Print 12th Edition (Elsevier). 2016.
- Lapić, I., Piva, E., Spolaore, F., Tosato, F., Pelloso, M., & Plebani, M. (2019). Automated measurement of the erythrocyte sedimentation rate: method validation and comparison. Clinical chemistry and laboratory medicine, 57(9), 1364–1373. https://doi.org/10.1515/cclm-2019-0204
- Orr, C. K., Najm, A., Young, F., McGarry, T., Biniecka, M., Fearon, U., & Veale, D. J. (2018). The Utility and Limitations of CRP, ESR and DAS28-CRP in Appraising Disease Activity in Rheumatoid Arthritis. Frontiers in medicine, 5, 185. https://doi.org/10.3389/fmed.2018.00185